What is Prolotherapy?
Call NOW
+ 359 889 159 302
About the therapy
The disturbances in the lives of people suffering from joint and back pain can be serious – from skipping work to reduced mobility. Prolotherapy uses the body’s natural healing ability to relieve chronic pain, strengthen damaged tissues and restore function. It is a procedure in which a naturally occurring irritant is injected into the soft tissues of a damaged joint or area. This deliberate inflammation is intended to signal the body that there is a problem, so our own body can cope with the construction of new tissues. This can provide significant relief for joint or back pain.
The treatment dates back to the 1930s, when Dr. Earl Gedney, an osteopath, a surgeon, has successfully used it to treat severe injuries to her own hands. Shortly thereafter, doctors Hackett and Hemwall perfected the therapy, and today it is widely used by many physicians as a way to deal with pain in the long term.


How does prolotherapy work?
Prolotherapy involves an injection that contains a natural irritant. This irritant may include:
- sugar (dextrose or glucose) alone or in combination with glycerol and phenol,
- sodium morphate (purified derivative of cod liver oil),
- sarapin (sterile aqueous solution of soluble salts of the plant Sarracenia purpurea and benzyl alcohol 0.75% or saline).
Usually, the selected substance is combined with a local anesthetic (lidocaine, procaine or martin).
The irritant is thought to stimulate the body’s healing response, creating localized, temporary inflammation. Inflammation activates fibroblasts (cells that produce collagen) and attracts platelets and stem cells to the area. Platelets provide many types of growth factors that have been shown to stimulate the formation of new blood vessels, activate more fibroblasts and deliver more stem cells to the affected area to heal the injection site.
Once activated, the body’s defenses and healing powers will begin to strengthen and repair the damaged tissues. When it comes to joints, strengthening the connections in the area helps stabilize the joint over time and relieve the pain.
Various types of prolotherapy are known: prolotherapy with dextrose, plasma prolotherapy including autologous, platelet-rich plasma (referred to as “PRP”) or bone marrow and / or adipose tissue that contain mature stem cells (known as bioterpules).
Which cases is prolotherapy good for?
Doctors use it most often in patients with back pain associated with sprains, stretching of ligaments and tendons. Suitable for prolotherapy are people with back pain who:
- have tendon or joint pain or weakness lasting more than 6 weeks;
- receive only temporary relief from manual or physical therapy;
- have undergone surgery without subsequent relief of back pain;
- have joint pain, which exacerbates when stressed and decreases when resting.
Prolotherapy is also applicable in the area of the knee, hip and shoulder joints and connecting tissues. Indications that this kind of therapy is needed may include: sciatica, back pain, torn meniscus, distended tendons and ligaments, neck pain, rotator cuff disorders, tennis elbow, chest pain, leg pain and more. In some cases, people with chronic illnesses, such as degenerative disc disease or arthritis, may use prolotherapy to relieve the pain.

What does the procedure include?
If a person is taking anti-inflammatory drugs, he or she should stop taking them 2 to 3 days before the procedure, as taking anti-inflammatory drugs may interfere with the effectiveness of the procedure.
On the day of the procedure, it is important for the person to eat well. Often, doctors recommend that a person undergoing prolotherapy should focus on protein-rich foods.
During the procedure, the skin is pre-treated with an alcohol or other sterilizing solution. A local anesthetic can then be applied to the skin to reduce discomfort at the injection site. In extreme cases, when the person is experiencing significant pain or discomfort, additional sedation may be used.
The procedure itself involves injecting the irritant solution with a long, thin needle at several different points around the target area of the back or joint. The number of injections used depends on the area or joints involved. Effects may require several injections at the site of injury or weakened area per session and several sessions over 3 to 6 months. The injection should be accurate so that the irritant is placed in the area or areas requiring recovery.
What are ligaments ?
Ligaments help to provide stability to joints. They prevent the joint from moving more than a normal range (though what is ‘normal’ varies from one individual to another). Some people have lax ligaments that allow more than ‘normal’ movement: often spoken of as ‘double jointed’ or hyper-mobile. In the spine there is a complex arrangement of ligaments, both between each vertebral segment and between the spine and pelvis, which allows flexibility in some directions and produces restraint in others.
Sometimes ligaments can be overstretched, or even torn (as in a sprained ankle). The ligament may then not control the joint adequately – thus leading to ‘instability’ which may put abnormal stresses on the joints and discs in the spine. The instability is compounded by breakdown in the muscle stabilising system through muscle weakness, fatigue and poor coordination.
In women, the pelvic joints need to be supple for child bearing, and so the ligaments soften and stretch more readily. Sometimes they do not tighten up after childbirth and therefore allow too much movement: hence ‘sacroiliac instability’.
It is good to know
Not all cases are appropriate for the procedure. Sometimes, in serious chronic conditions, there may be no effect, so the doctor may suggest other alternatives.
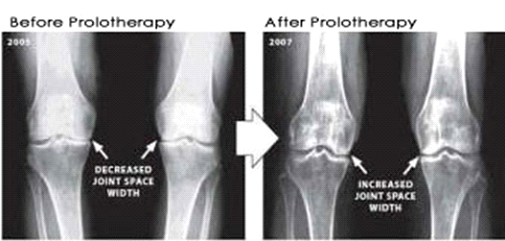
X-ray or other types of imaging may sometimes be necessary to assist in assessing the need and ability to perform the procedure, taking into account the location and severity of the injury.
Many medical professionals around the world believe this is a safe alternative or additional treatment for back and joint pain.
What we have achieved so far
0
Years of practice worldwide
0
Countries worldwide
0
+
Satisfied patients worldwide
0
Years practice in Bulgaria
0
+
Satisfied Bulgarians